Contact Allergens: Patch Testing and Common Irritants
If you’ve had a stubborn rash that keeps coming back no matter what creams you use, you’re not alone. Many people assume it’s just dry skin or a reaction to soap-but sometimes, the real culprit is something you’re touching every day. That’s where patch testing comes in. It’s not a quick fix, but it’s the most reliable way to find out exactly what’s triggering your skin flare-ups. Unlike regular allergy tests that check for reactions to pollen or food, patch testing looks at the chemicals in your shampoo, jewelry, clothing, or even your phone case that your immune system has learned to hate over time.
What Is Patch Testing?
Imagine sticking small patches of tape on your back, each holding a tiny drop of a different chemical. You wear them for two full days without getting them wet. Then, a few days later, your doctor checks for redness, bumps, or blisters where those patches sat. That’s patch testing. It’s not painful, but it’s annoying-you can’t sweat, shower, or even wear a tight shirt. But if you’ve been struggling with a rash for months, it’s worth it.
This test isn’t designed to catch immediate reactions like hives or sneezing. Instead, it finds delayed allergic reactions, which take 48 to 96 hours to show up. These are called type IV hypersensitivity reactions, and they’re behind most cases of allergic contact dermatitis. That’s the medical term for when your skin gets inflamed because your immune system recognizes a substance as a threat-even if it’s harmless to everyone else.
Doctors use this test because it’s the only method that reliably identifies these delayed reactions. Skin prick tests, which are common for food or pollen allergies, won’t work here. They look for immediate, IgE-mediated responses. Patch testing? It’s all about T-cells and slow-burning inflammation.
How It Works: Step by Step
The process usually takes about a week and involves three visits to the dermatologist’s office.
- Day 1 (Application): Small aluminum chambers, called Finn chambers, are attached to your back using adhesive tape. Each chamber holds one allergen-anything from nickel to fragrances to preservatives. You might get 30 to 100 different substances tested at once. The allergens are mixed with a special white petrolatum base to ensure they’re at the right concentration to trigger a reaction without burning your skin.
- Day 3 (Removal): After 48 hours, you return. The patches are gently peeled off. Your skin might look red or irritated already, but that doesn’t mean anything yet. The doctor marks exactly where each patch was so they can check later.
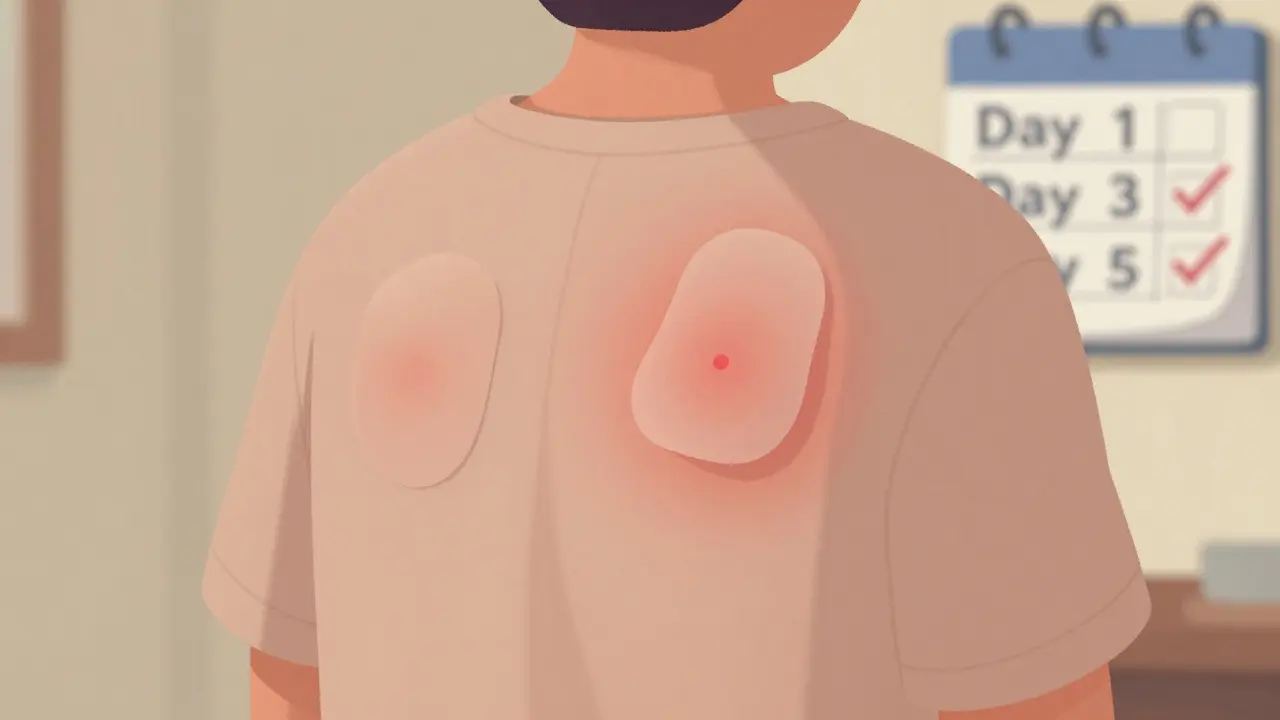
- Day 5 (Reading): Two days after removal, you come back again. This is when the real results show up. A positive reaction looks like a raised, red, itchy bump right under where the patch was. Some reactions are subtle-just a slight darkening of the skin. Others are dramatic. The doctor compares your skin’s response to a standard scale to determine if it’s a clear allergic reaction.
During those 48 hours, you can’t get the patches wet. No showers, no swimming, no heavy sweating. Even a little moisture can wash away the allergens or cause false results. Some people find it hard to sleep without rubbing the patches off. Others can’t wear a bra or tight shirt. It’s uncomfortable, but skipping these rules makes the whole test useless.
Common Contact Allergens
There are thousands of possible allergens, but a handful show up again and again in patch tests. Here are the most common ones:
- Nickel: Found in jewelry, belt buckles, zippers, coins, and even some eyeglass frames. It’s the #1 allergen worldwide. Even a small amount from a cheap earring can trigger a reaction.
- Chromates: Used in cement, leather tanning, and some paints. Construction workers and mechanics often test positive.
- Formaldehyde and formaldehyde-releasing preservatives: These hide in shampoos, lotions, baby wipes, and even some makeup. They’re added to stop bacteria from growing, but for sensitive skin, they’re a disaster.
- Neomycin: A common ingredient in antibiotic ointments. Ironically, the cream meant to heal your skin can make it worse if you’re allergic.
- Quaternium-15: Another preservative found in cosmetics and personal care products. It’s sneaky because it’s not always listed clearly on labels.
- Perfumes and fragrances: Even “unscented” products can contain masking fragrances. Natural scents like lavender or tea tree oil can trigger reactions too.
- Parthenolide: Found in chamomile and daisies. Florists and gardeners often test positive for this one.
- Epichlorohydrin: Used in epoxy resins. People who do home repairs or work with adhesives are at risk.
These are just the usual suspects. But your job, if you’re diagnosed with an allergy, is to find out what’s in your everyday products. Read labels. Look for ingredient names, not just “fragrance.” Some allergens are listed under chemical names you’ve never heard of. That’s why knowing your trigger is only half the battle.
What Patch Testing Can’t Do
It’s important to understand the limits. Patch testing doesn’t catch everything. For one, it only tests for substances included in the panel. A standard panel covers about 70% of cases. An expanded panel-used for people with occupational exposure, like dental workers or hairdressers-can catch up to 80%. But there are still thousands of chemicals out there that aren’t tested.
Also, a negative result doesn’t mean your rash isn’t caused by contact. Sometimes, it’s irritant contact dermatitis-not allergic. That’s when a substance like bleach, detergent, or even repeated handwashing damages your skin directly, without involving your immune system. Patch testing won’t pick that up. Your doctor will need to look at your history, your job, and your habits to figure it out.
And sometimes, even if you test positive, you might not realize you’re being exposed. Maybe you’ve been using the same lotion for years. Maybe your new phone case has a coating that contains nickel. Or maybe your partner’s shampoo is transferring allergens to your pillowcase. Identifying the trigger is only the first step. Avoiding it takes work.
What Happens After a Positive Result?
Once you know what you’re allergic to, the treatment isn’t a pill-it’s lifestyle changes.
- Avoidance: This is the most important step. If you’re allergic to nickel, stop wearing cheap jewelry. Use plastic or coated zippers. Look for products labeled “nickel-free.”
- Switch products: Replace your shampoo, lotion, or detergent with ones that don’t contain your allergens. Look for fragrance-free, preservative-free options. Brands like CeraVe, Vanicream, and Aveeno’s Free & Clear line are often recommended.
- Treat the inflammation: Your doctor may prescribe a mild topical steroid cream to calm down the rash. For severe cases, a short course of oral steroids might be needed.
- Manage itching: Antihistamines won’t stop the allergic reaction itself, but they can help with the itch. You can keep taking them during patch testing-unlike with other allergy tests, they don’t interfere.
- Use barrier protection: If you can’t avoid exposure (like if you work with chemicals), wear gloves or protective clothing. Cotton under gloves helps absorb sweat and reduces irritation.
Education is key. Dermatologists at UC Davis Health and the University of Michigan both stress that knowing your triggers allows you to avoid them-and that’s how you prevent future flare-ups. One patient might learn they’re allergic to a preservative in their moisturizer. Another might find out their work boots contain a chemical they’ve been exposed to for years. The relief isn’t instant, but it’s lasting.
What If the Test Is Negative?
If your patch test comes back negative, don’t give up. Your rash might still be caused by contact-but not in the way the test looks for. Here’s what to try next:
- Repeat testing: Sometimes, a second round with an expanded panel picks up something the first one missed.
- Repeat open application test: This is a DIY version you can do at home. Take a small amount of the product you suspect (like your hand soap) and apply it to a 2-inch patch of skin on your forearm twice a day for 5-10 days. If you don’t get redness or itching, it’s probably not the culprit. If you do, you’ve found your trigger.
- Check for irritants: Think about frequency of washing, water temperature, harsh soaps, or even friction from clothing. Irritant dermatitis is super common and often mistaken for allergy.
- Consider other causes: Eczema, psoriasis, fungal infections, or even stress can mimic contact dermatitis. A dermatologist can help rule those out.
Why This Matters
Contact dermatitis isn’t just a nuisance. It can turn into a chronic condition that affects sleep, work, and confidence. A rash on your hands can make it hard to type. One on your face can make you avoid mirrors. Left untreated, it can lead to infections or scarring.
But here’s the good news: once you know what’s causing it, you can take control. You don’t have to guess anymore. You don’t have to try every cream on the shelf. You can make smart, informed choices about what you put on your skin.
That’s the power of patch testing. It’s not glamorous. It’s not quick. But for people who’ve spent years chasing answers, it’s the closest thing to a cure there is.
Can I do patch testing at home?
No, patch testing should only be done by a trained dermatologist. The allergens used are highly controlled, and the interpretation of results requires expertise. DIY tests or over-the-counter kits are unreliable and can cause false reactions or even skin damage.
Do I need to stop using my medications before patch testing?
No. Unlike skin prick tests, patch testing is not affected by antihistamines or most other allergy medications. You can keep taking them. However, if you’re on oral steroids, your doctor may ask you to pause them a week before the test, as they can suppress the immune response and lead to false negatives.
How long do the results last?
Allergies identified through patch testing are usually lifelong. Once your immune system recognizes a substance as a threat, it tends to remember it. Avoiding the allergen is the best way to prevent future reactions. Re-exposure can cause a reaction even years later.
Can patch testing help with eczema?
Yes-if your eczema is worsened by contact allergens. Many people with atopic dermatitis (eczema) also have allergic contact dermatitis. Identifying and avoiding triggers can significantly improve skin condition. Patch testing helps differentiate between general eczema and allergy-driven flare-ups.
Is patch testing covered by insurance?
Most insurance plans cover patch testing when ordered by a dermatologist for suspected allergic contact dermatitis. However, coverage depends on your plan and whether you’ve tried other treatments first. Always check with your provider before scheduling.
If you’ve been dealing with a mysterious rash for months, patch testing could be the missing piece. It’s not about finding a quick cure-it’s about finding the truth. And once you know what’s causing your skin to react, you can finally stop guessing and start living without it.

10 Comments
Patch testing saved my life. Had a rash for 3 years. Turned out it was nickel in my watchband. Ditched the watch. Skin cleared in a week. Stop guessing. Get tested.
i did this test last year and it was such a pain in the ass no showering for 2 days?? i just wore a tank top and tried not to move. also my doctor used like 50 patches and my back looked like a zombie had chewed on it lol
You're not alone! I was terrified to do this but it was the best decision I ever made. My dermatologist was so patient and explained everything. You've got this!
Important note: formaldehyde-releasing preservatives are everywhere. Look for DMDM hydantoin, imidazolidinyl urea, and quaternium-15 on labels. They're silent killers. I switched to preservative-free brands and my eczema vanished. Also, avoid baby wipes-they're loaded.
I cried when I found out it was my phone case. 😭 Like... my PHONE. The thing I touch 200 times a day. I thought I was being dramatic until my skin literally screamed at me. Now I use a silicone case. My back is healing. I feel like a new person. 🙌
Patch testing is a scam. Big Pharma wants you to think it's science. The real cause? EMFs from your devices. Your skin is reacting to Wi-Fi. They don't test for that. They don't want you to know. Go off-grid. Live in a cabin. Your skin will thank you.
This whole thing is overblown. I had a rash for 6 months. Tried patch testing. Negative. Then I stopped using soap. Just water. Done. Problem solved. You people overthink everything. It's not a conspiracy. It's just soap.
In occupational dermatology, chromate exposure in cement workers is a well-documented hazard. Standard patch panels omit industry-specific allergens. Recommend extended panels for construction, leather, and metalworking industries. Prevention > diagnosis.
I did this test and it was a waste. Turned out I was allergic to my own sweat. Which is basically just... me. So now I have to live in a climate-controlled room? That's not a solution. That's a prison.
Actually, I got a positive for parthenolide but I don't even own chamomile tea. Then I found out my cat licks chamomile wipes and sleeps on my pillow. So it's not me. It's my cat. Who knew?